March 10, 2014 is National Women and Girls HIV/AIDS Awareness Day (NWGHAAD). NWGHAAD is a nationwide effort to help women and girls take action to protect themselves and their partners from HIV – through prevention, testing and treatment. The HIV epidemic is rapidly aging with 17% of new HIV diagnoses in the U.S. occurring in those 50 and older. By 2015 the CDC expects half of the HIV infected population to be over 50. Older Americans are more likely than younger Americans to be diagnosed with HIV at a later stage in the disease. This can lead to poorer diagnoses and shorter HIV to AIDS intervals. And with HIV and age, comes cancer.
Statistics – An Overview
- One in four people living with HIV infection in the U.S. are women.
- According to the CDC, 275,700 American women are living with HIV/AIDS.
- Women made up 20% (9,500) of the estimated 47,500 new HIV infections in the U.S. in 2010 with most (84%) of these new infections in women being from heterosexual contact.
- 4,014 women with an AIDS diagnosis died in 2010 and an estimated 111,940 women have died since the beginning of the epidemic.
- Only 41% of HIV positive women are retained in HIV related medical care and only 26% of HIV positive women achieve viral suppression. Viral suppression improves survival and reduces transmission to others.
Disproportionate Affect on Women of Color
-
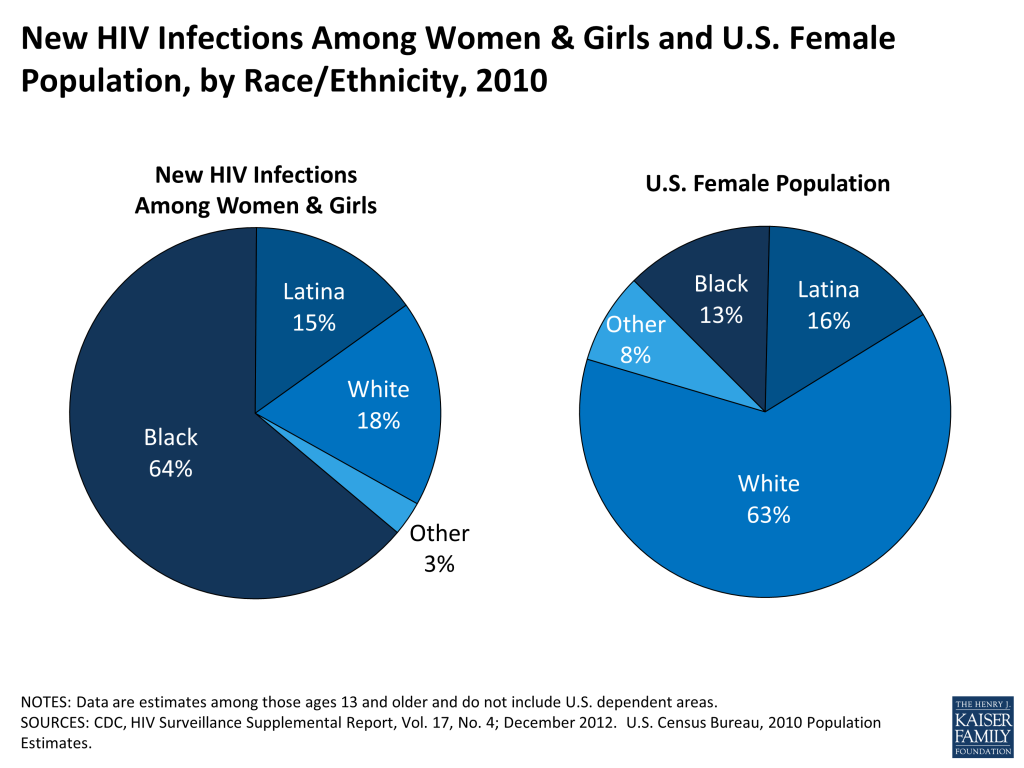
- Black and Hispanic women continue to be disproportionately affected by HIV, compared with women of other ethnicities.
- While only 13% of the U.S. female population, Black women represent 64% of new female HIV infections.
- At some point in their lifetimes, an estimated 1 in 32 African American women will be diagnosed with HIV infection.
- Some good news: While African American women accounted for almost two-thirds of all estimated new HIV infections among women in 2010, there was a 21% decrease in new HIV infections between 2008 and 2010.
- By the end of 2010, Hispanic women had an HIV infection rate more than four times that of white women. Hispanic women represented 15% of new HIV infections among women and 19% of all women living with HIV.
Reasons Women are Affected by HIV
- Some women may be unaware of their male partner’s risk factors for HIV (such as injection drug use or having sex with other men) and may not use condoms
- Women have a much higher risk for getting HIV during vaginal sex without a condom than men do.
- For older women, the physical changes of aging such as vaginal drying and the thinning of the vaginal wall due to a loss of estrogen can increase a woman’s susceptibility to HIV and other STDs.
- Some sexually transmitted infections, such as gonorrhea and syphilis, greatly increase the likelihood of getting or spreading HIV. STIs are much more prevalent in Black and Hispanic communities. For instance in 2011, Blacks had 17 times the reported gonorrhea rates of whites.
- Women may be afraid that their partner will leave them or even physically abuse them if they try to talk about condom use.
- Women who have been sexually abused may be more likely than women with no abuse history to engage in sexual behaviors like exchanging sex for drugs, having multiple partners, or having sex with a partner who is physically abusive when asked to use a condom.
- Some HIV infections among women are due to injection drug and other substance use—either directly (sharing drug injection equipment contaminated with HIV) or indirectly (engaging in high-risk behaviors while under the influence of drugs or alcohol).
- The higher proportion of people living with HIV in many Black and Hispanic communities means individuals in those communities face a greater risk of infection with every sexual encounter.
HIV and Cancer Risks
- People infected with HIV have a higher risk of some types of cancer than uninfected people.
- A HIV weakened immune system; infection with other viruses such as HPV, Hepatitis B or C and Epstein Barr; and traditional risk factors such as smoking all contribute to this higher cancer risk.
- HIV treatments have greatly reduced the incidence of AIDS defining cancers such as Kaposi’s sarcoma and non-Hodgkin’s lymphoma as compared to the early years of the epidemic.
- However, various other types of cancers are much more likely to develop in people with HIV. These cancers include anal cancer (10+ times as likely); Hodgkin’s lymphoma (10-20x); head, neck and liver cancers (8-10x); cervical cancer (5-8x); and lung cancer (2.5-7.5x)
- Except for Hodgkin’s lymphoma, these cancers are diagnosed on average 10-15 years earlier in HIV+ people compared to the general population.
- The story is not all bad. People infected with HIV do not have increased risks of breact, colorectal, prostrate or many other common types of cancer.
- What can be done:
- Successful HIV treatment can reduce cancer rates up to 50%.
- Screening for HPV, anal cancer and cervical cancer.
- Tobacco use in people living with HIV/AIDS runs 2-3 times the national average. Reduce smoking to reduce rates of lung, throat, and mouth cancers.
- Diet and exercise as well as reduced alcohol and substance use.
- For those co-infected with Hepatitis B or C, successful Hepatitis treatment reduces liver cancer rates.
How to help
- Increase awareness of safe practices to prevent HIV infection.
- Encourage women to get tested and to know their status and the status of their partners. Find a place to get tested.
- Link HIV+ women to HIV medical care and help them overcome barriers to getting care.
- For those without health care, the Affordable Care Act makes it easier for HIV positive women to receive the care they need. Under the ACA, a woman with a pre-existing condition, such as HIV/AIDS, can no longer be denied insurance because of her health status. People with low and middle income may be eligible for tax subsides that will help them buy coverage. Open enrollment for 2014 ends March 31. Apply for coverage now.
- Encourage women to stay in care and achieve “viral suppression” by using treatment to keep HIV at a level that helps individuals stay healthy and reduces the risk of transmitting the virus to others.
Patrick Aitcheson is the Communications and Logistics Administrator for the Diverse Elders Coalition (DEC). The opinions expressed in this article are those of the author and do not necessarily reflect those of the Diverse Elders Coalition.