 Earlier this week, I had the honor of being a panelist at an “Adult Vaccines Save Lives” briefing on Capitol Hill to help launch the Adult Vaccine Access Coalition. The Coalition brings together leaders in health and public health to raise awareness and engage in advocacy on the importance of adult immunization. With the aging of the U.S. population, the public health impact of vaccine-preventable diseases and their complications in older adults is likely to grow.
Earlier this week, I had the honor of being a panelist at an “Adult Vaccines Save Lives” briefing on Capitol Hill to help launch the Adult Vaccine Access Coalition. The Coalition brings together leaders in health and public health to raise awareness and engage in advocacy on the importance of adult immunization. With the aging of the U.S. population, the public health impact of vaccine-preventable diseases and their complications in older adults is likely to grow.
Why Should We Vaccinate Older Adults?
The diminishing function of the aging immune system reduces the immune response to vaccination and underscores the need to develop more effective products for older adults. People age 65 years and older account for a disproportionate amount of morbidity and mortality from vaccine-preventable diseases, especially from influenza, pneumococcal disease, and shingles. Older adults who reside in long-term care and assisted living facilities are at risk for outbreaks of vaccine-preventable diseases, and in particular influenza, as they often have lower vaccine coverage levels than persons living in community settings.
The Relationship Between Chronic Conditions and Vaccinations
Adults with chronic conditions – such as asthma, COPD, diabetes, and heart disease – are more likely to develop complications from certain vaccine-preventable diseases, including long-term illness, hospitalization, and even death. The CDC estimates that among US adults each year there are approximately 40,000 cases and 4,000 deaths attributable to invasive pneumococcal disease, between 3,000 and 50,000 deaths are due to seasonal influenza, 9,000 cases of pertussis, approximately 3,000 cases of acute hepatitis B, and about one million cases of herpes zoster. The Advisory Committee for Immunization Practices (ACIP) recommends that older adults should receive annual influenza vaccination, one dose each of pneumococcal conjugate and pneumococcal polysaccharide vaccine, and one dose of zoster and Tdap vaccines if they have not previously received them. Other vaccines, such as hepatitis A and B and meningococcal conjugate may also be needed, depending on the person’s health and other factors. For many diverse elders, however, these necessary vaccines may be out of reach.
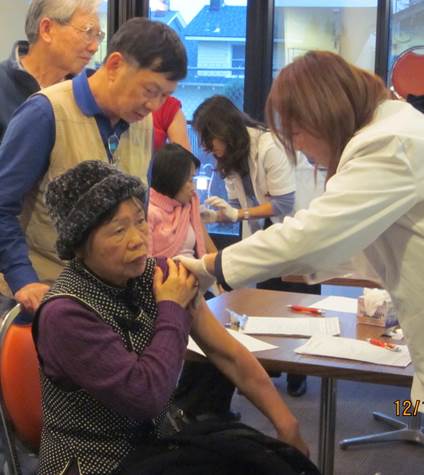
Barriers to Accessing Vaccinations
Several system barriers, including lack of proper health insurance and vaccination costs, limit access to adult vaccinations for diverse elders. For Asian Americans and Pacific Islander (AAPI) older adults, the number of those uninsured far exceeds the national rate. Seven out of the top 10 uninsured ethnic groups in the US are AAPIs.
Many AAPI older adults do not have Medicare, either, partly due to immigration. Without Medicare or private insurance which covers much of the costs associated with vaccinations, AAPI older adults may be unable to afford the vaccinations.
For those who do have Medicare, despite coverage of many adult vaccinations, the variation in coverage is of particular concern. As mentioned above, Tetanus and Shingles vaccines are recommended to all older adults by the ACIP, and yet, the Shingles vaccination is only covered by Medicare Part D. This can result in a financial barrier, as many Medicare Part D plans charge a co-payment or require the patient to pay for the vaccination upfront and bill the drug plan for repayment. As a prescription drug benefit, Part D was designed to be implemented by pharmacists. Due to this design, it is difficult for physicians to provide vaccines covered under Part D in their offices.
Other systems issues that create barriers for diverse elders to access needed vaccines include lacking or underuse of administrative systems (e.g. electronic medical records); concerns about reimbursement/ administration fees paid by health insurers, which can discourage providers from stocking all adult vaccines; and, lack of integration of vaccines into adult medical care.
 Cultural and educational barriers also prevent AAPI elders from getting needed vaccines. Many people choose not to get vaccinated because they don’t believe they need it; they may believe that they can prevent the disease or have skepticism about the vaccination’s safety.
Cultural and educational barriers also prevent AAPI elders from getting needed vaccines. Many people choose not to get vaccinated because they don’t believe they need it; they may believe that they can prevent the disease or have skepticism about the vaccination’s safety.
New immigrants are generally unfamiliar with the US healthcare system and have a limited knowledge of preventive medicine and disease monitoring. Additionally, providers may not be aware of barriers among AAPI immigrants, such as the elevated risk for Hepatitis B. Without in-language information available, older adults with limited-English proficiency (LEP) are unable to access the necessary information to make an informed decision about vaccinations. Additional cultural and language barriers may include confusion about how to use care when insured; perceived stigma; understanding who is at risk; and incorrect beliefs about preventive care.
Solutions
Adult vaccine education, provision and coverage plans must reflect our nation’s growing diversity, and strategies to increase adult vaccination should first look to the barriers faced by many older adults. To learn more about the federal initiatives to increase adult vaccinations, you can visit the National Adult Vaccination Program’s website at www.navp.org. For more information about the Adult Vaccine Access Coalition, visit www.adultvaccinesnow.org.
The opinions expressed in this article are those of the author and do not necessarily reflect those of the Diverse Elders Coalition.

