by John-Manuel Andriote. This article originally appeared on Next Avenue.
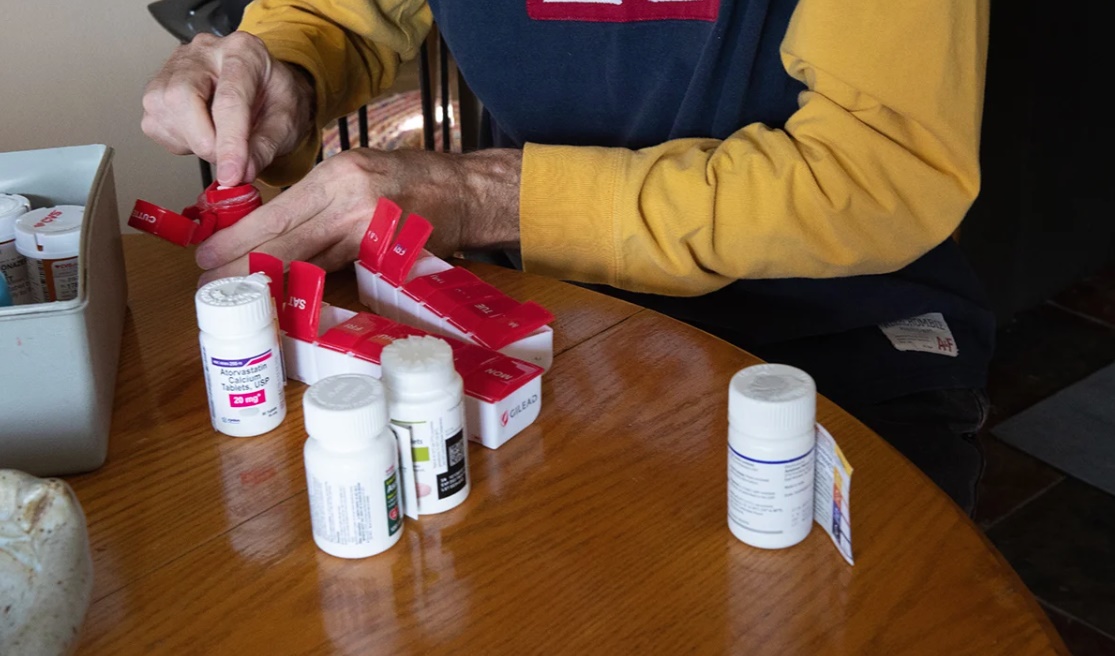
Credit: Bridget Caswell
Craig Washington has never spent a night in the hospital because of HIV. Not even the time in the early ’90s when he got cryptosporidiosis, one of the opportunistic infections that can wreak havoc on someone with a weakened immune system.
The Atlanta-based social worker and therapist’s good health is especially impressive for a 60-year-old man diagnosed with HIV back in 1985 — the year the HIV antibody test first became available.

60-year-old Craig Washington of Atlanta, who has lived with HIV since 1985. (Photo courtesy of Craig Washington)
“For the most part,” said Washington, “I have been very blessed, very fortunate, that my health is pretty good and a lot of the day-to-day energy level I’ve been able to sustain.” He attributes his good fortune to his doctors, regular exercise and a support network of friends.
Washington says his ability to continue working, and thereby remain continually insured, provides a level of continuity in his health care that many people living with HIV/AIDS don’t have.
Diagnosed in 1992, 53-year-old Michael Luciano’s reality is very different.
The New York City native now living in Charleston, S.C. returned to the workforce three years ago after spending 24 years on disability. Today, he holds a two-thirds-time job as a treatment educator for Palmetto Community Care, an HIV services organization in Charleston.
“I stayed on disability and felt trapped there because the thought of going off disability and finding a job locally that would pay enough for co-pays and insurance paralyzed me,” Luciano said. Although his job provides “not the greatest” insurance coverage, Luciano hopes this position lasts — or another one arises that would help him stay off disability. “I sort of lucked into a position that worked out for me,” he said.
But it’s not only a matter of job security. Luciano wonders how long he will be able to continue working. Although he manages HIV with medication, other chronic conditions he’s developed over the years give him trouble.

Charleston, S.C.-based, 53-year-old Michael Luciano was diagnosed with HIV in 1992. (Photo courtesy of Michael Luciano)
“One of my major, ongoing challenges — and that makes me anxious about continuing working to retirement age — is osteoarthritis in my hands and both knees,” he said.
Even after finally beginning to manage with medication the rheumatoid arthritis in his hands, Luciano’s severe osteoarthritis makes exercise virtually impossible. “Osteoarthritis presented much earlier than expected,” he said. “It’s a classic symptom of advanced HIV infection and has had secondary impacts on my health.”
He also experiences kidney dysfunction due to the HIV drugs. There’s bone density loss. And on top of it all, Luciano said, there is the “ongoing level of anxiety it generates for my future as I approach the age when all of these conditions manifest.”
If that’s not enough to make someone worry about aging with HIV/AIDS, there are also financial concerns (medications and frequent medical visits aren’t cheap), not to mention managing mental health. “[Mental health] is intimately tied to physical health,” Luciano said. He occasionally finds himself “overwhelmed by anxiety or depression.”
Luciano’s experience is much like that of many long-term HIV/AIDS survivors — those diagnosed before effective treatment became available in 1996, as defined by long-term survivor Jésus Heberto Guillen Solis, founder of the nearly 5,000-member HIV Long-Term Survivors group on Facebook.
Aging Ahead of Their Time?
It’s not yet clear to researchers how HIV/AIDS and the natural aging process interact — mainly because the first people ever to age with HIV are in the process of doing so. For this reason, debate rages as to whether people living with HIV/AIDS are prone to so-called “accelerated aging,” and, if not, who is most vulnerable, what causes it and what might be done to slow it down.
Even “normal” aging involves losing muscle mass, bone loss, weight loss, memory loss, decreased kidney, brain and heart function and a deteriorating immune system. Many factors, both genetic and environmental, affect its pace from one person to another.
Medical research on aging with HIV/AIDS can seem contradictory. One study says accelerated aging is real and that getting older with HIV/AIDS seems to inevitably bring on conditions and diseases usually seen only in much older people. Another says it’s not really accelerated but only accentuated — that medically-controlled HIV/AIDS is only one of the conditions inflicting harm. Myocardial infarction or end-stage renal disease, for example, in anyone with the same overall profile, is different only in their HIV status.
Monty Montano, assistant professor of medicine at Harvard Medical School, scientific director of the Boston Pepper Center at Brigham and Women’s Hospital and researcher on chronic HIV, prefers the term “asynchronous” to “accelerated” to describe HIV/AIDS’ effects on aging.
“Think of a concert, a symphony, with a large orchestra,” Montano said. “Each instrument plays its role. But if one section of the symphony is playing at the wrong time — too early or too long — it creates an asynchronous progression.”
In other words, some of the common effects we associate with older age may be present in an HIV-positive individual in their 40s or 50s, but not all of them. So while some things may be off-kilter (high blood pressure or osteoarthritis, say), the overall picture isn’t that of an “old” person.
To an extent, it’s semantics, as researchers are trying to explain why so many people aging with HIV/AIDS experience what we think of as aging-associated conditions at an earlier age. It’s also a matter of teasing out precisely what is meant by whichever words (accelerated, asynchronous, accentuated, age advancement, etc.) are used and avoiding generalizing findings of limited research studies to the millions of people living with HIV/AIDS.
Current Research Says…
A 2019 study reported in the journal AIDS found there wasn’t a significant difference between treated HIV-positive and HIV-negative individuals when considering 10 biomarkers that are used as measures of biological age. The researchers compared HIV-positive and HIV-negative individuals with similar age, sex, years of education, cigarette smoking and recreational drug use to gauge what they called “age advancement” by subtracting their chronological age from their biological age.
They found that ethnicity, sexual orientation or lifestyle factors such as smoking cigarettes or using recreational drugs apparently didn’t matter. What did matter for both the HIV-positives and negatives was having cytomegalovirus (CMV), chronic hepatitis B virus (HBV), CD4 and CD8 white blood cell counts and their ratio to each other; time since HIV diagnosis; the lowest CD4 cell count below 200/mm3 (the normal range is 500-1,400) and how long someone was on anti-HIV medications.
The study also implicated some of the older HIV/AIDS drugs, particularly saquinavir, the first protease inhibitor drug approved in 1995 to be used in the “combination therapy” that marked a dramatic turning point in the HIV/AIDS epidemic when it became possible to live with the virus rather than almost inevitably progress to AIDS and die. Many long-term survivors took saquinavir when it was first approved, combined with other drugs in the so-called “cocktail.” Research suggests saquinavir had significant negative long-term effects in those who took it. That’s one reason it is no longer used as a first-line HIV treatment.
These researchers concluded that people with managed, undetectable HIV viral loads “may experience accentuated aging compared with HIV-negative individuals with similar lifestyles” based on the set of biomarkers they used to measure aging. “This age advancement appears to be related to viral co-infections such as CMV and chronic HBV, but also to historic severe immunosuppression and possibly exposure to particular antiretroviral drugs,” they wrote.
A 2014 study of 98,687 male American military veterans — 31% HIV-positive, 69% HIV-negative — supports the idea of “accentuated” aging for HIV-positive people, but not “accelerated” aging. The study, reported in the journal Clinical Infectious Disease, found that HIV-positive and negative men, who had traditional risk factors such as diabetes or high cholesterol, were at heightened risk and developed such aging-associated conditions as myocardial infarction, end-stage renal disease and cancers not related to HIV at about the same age. They did not occur earlier in the HIV-positive participants.
“Our data show that HIV is a risk factor for these outcomes,” wrote the researchers in their report, “however, many traditional risk factors have a similar or greater magnitude of relationship with these outcomes.” They suggested that targeting those risk factors “may help decrease the excess burden of aging-related diseases among HIV-infected adults.” They added, “These findings should reassure HIV-infected patients that they are unlikely to experience these conditions decades earlier than those aging without HIV.”
But what of those people aging with HIV/AIDS who are experiencing conditions — like Luciano’s severe osteoarthritis — that seem to have arisen so much earlier than typically seen in HIV-negative people?
“No two individuals who have HIV or not are likely to age exactly the same way,” said Dr. Amy Justice, Long Professor of Medicine at Yale University, clinical epidemiologist and one of the researchers on the 2014 veterans study. “We bring our individual exposures and genetics and lifestyles to the table — the prior slings and arrows that we have experienced. And one of those slings and arrows can be HIV infection.”
Justice added that people treated with earlier, partially-effective HIV medications are likely to have a different experience than those who receive treatment at an earlier stage of the infection. But even with today’s highly-effective HIV treatments, Justice said, “It’s not as though we can wipe away all the effects of HIV.” She explained that even with well-managed HIV, “there is still likely to be some effect because we’re not curing folks.”
Of course there are still those other “slings and arrows” that affect our health no matter our HIV status. That’s why Justice gives the same advice to anyone over age 65, with or without HIV/AIDS: exercise, eat well, either don’t smoke or stop smoking tobacco, use alcohol modestly, think carefully about all the medications and supplements you take and have a good doctor.
Boring Isn’t Bad
It also helps to be what Harold R. “Scottie” Scott of Lebanon, Tenn. calls himself: the most boring patient.

Harold R. “Scottie” Scott of Lebanon, Tenn. calls himself “the most boring” HIV/AIDS patient. (Photo courtesy of Harold Scott)
“I’ve never done drugs, have an occasional drink and smoked pot once,” Scott, who was diagnosed in 1991 said.
At 58, Scott is dealing with high blood pressure and chronic kidney disease. He continues on disability because, he said, “I’m healthy enough to do some things, but not enough to go full force.”
Unfortunately, most HIV-positive people in the over-50 population don’t fit that definition of boring. They frequently experience polypharmacy, being on five or more non-HIV drugs. And with each additional medication comes an increased potential for adverse drug interactions. Studies find they are far likelier than the general population to be co-infected with either hepatitis B or C; have chronic human papillomavirus (HPV); are up to three times likelier to smoke cigarettes and have far higher rates of mental illness and substance abuse than people who don’t have HIV/AIDS.
Another important factor affecting aging and risk: inflammation. Even HIV-positive people with an undetectable viral load experience chronic, low-grade systemic inflammation. The immune system remains hyper-vigilant knowing there’s a hostile foreign presence in the body.
The result is what is referred to as “inflamm-aging,” a significant risk factor for illness and death in elders. Fundamentally, “inflammation is aging,” said Dorcas Baker, a research nurse at Johns Hopkins University in Baltimore and co-founder of a support group for HIV-positive women called Older Women Embracing Life (OWEL).
Since the immune system is centered in what we call the gut, it makes sense that keeping the gut as healthy as possible is essential to fighting inflammation. Although further research is needed, scientists have found intriguing connections between taking probiotics for a healthy gut and improved immune health.
“What we are now realizing is that HIV as a disease is really a disease of inflammation. We are looking at simple interventions to affect the immune system, so probiotics and prebiotics would be the way of modulating the gut microbiome, the inflammation, and then see the aging effects or the noncommunicable diseases being reduced,” said Alan Landay, chair of the immunology and microbiology department at Chicago’s Rush University Medical Center in an interview with SciDev.Net.
In the meantime, the good news for those aging with HIV/AIDS is that there already are well-known ways to make growing older with the virus as healthy an experience as it can be.
HIV-suppressing antiretroviral drugs are the first line of defense, dramatically reducing inflammation. “There is profound resolution of inflammation with treatment,” said Montano, adding, “but it’s still not back to normal.”
In Short: Don’t Generalize
Just as screens and blood tests present ranges of what is considered normal or not, it’s important to remember that aging with HIV/AIDS also presents a range of possible experiences that are affected and shaped by individual factors.
“This idea of aging needs to be reframed to what you define as a good quality of life for your life,” said Montano.
Mark Brennan-Ing, a senior research scientist focused on HIV and aging at Hunter College’s Brookdale Center for Healthy Aging in New York City, praised work like Justice’s with veterans that shows the spectrum of individual experiences with HIV, notably that “the HIV-positive and negative folks also share similar types of characteristics.” Broad-brushing everyone aging with HIV as all facing the same level of risk or complications “further stigmatizes HIV,” Brennan-Ing said.
Brennan-Ing, whose psychosocial research focuses on how vulnerable older adults cope and adapt to chronic conditions, said it’s important to “swat down” discussions veering toward suggesting that “accelerated” aging is inevitable simply because someone has HIV, that all people with HIV/AIDS will age the same way or that it will invariably mean aging poorly. “Growing older with HIV is hard enough,” said Brennan-Ing, “let alone exaggerating it with this.”
There may be something even more important to learn from people aging with the virus beyond its physiological effects. It’s impossible, after all, to consider “health” without factoring in mental health, financial health and a host of other factors that affect our overall health and well-being. “When we talk about long-term survivors,” says Brennan-Ing, “there is a degree of resilience and hardiness that has let people become long-term survivors. That is something to capitalize on.”

(Editor’s note: This story is part of Still Here, Still Positive: a series on the first generation of Americans aging with HIV/AIDS, with support from The John A. Hartford Foundation.)
The opinions expressed in this article are those of the author and do not necessarily reflect those of the Diverse Elders Coalition.
