By Renée Markus Hodin. This article originally appeared on Community Catalyst.
In January of this year, I traveled to upstate New York to help my very active 83-year-old father move into an independent living building. He had been contemplating this move for a few years since my mother’s passing in 2015, but had wrestled with the decision. What finally pushed him to make the move was his own realization that he needed and wanted more social engagement in his life. And for the first six weeks after his move, he took full advantage of the opportunity to easily enjoy meals with other residents and to participate in movies, lectures and other programming. So when the pandemic hit the Northeast in mid-March, he found himself in quickly shifting sands. First to go were his volunteer activities: no more delivering Meals on Wheels, no more transporting nursing home residents to physical therapy. Soon after that, his synagogue and the Jewish Community Center where he did his daily workouts shut down. His world was becoming smaller and smaller by the day, until the point at which his building fully locked down, prohibiting residents from leaving the building and largely confining them to their own apartments. My father was now shut off from seeing his neighbors, local family members and friends. Over the next few months, talking with him on the phone or video calls, I sensed that he was becoming – quite atypically for him – increasingly confused and distressed.
My father’s experience over the last seven months has largely mirrored those of tens of millions of older adults across the country, including many of those working with our advocacy partners. Even before the pandemic began, social isolation and loneliness were widespread among older adults. Approximately one-quarter of community-dwelling Americans aged 65 and older were considered to be socially isolated, and 43 percent of adults aged 60 and older reported feeling lonely. Indeed, a consensus study report from the National Academy of Medicine identified social isolation and loneliness as “serious public health risks.” As we noted back in March, social isolation has been associated with a whole host of poor health outcomes such as an increased risk of developing dementia, heart disease or depression and of premature death.
We’re only just beginning to understand the toll the pandemic is taking on older adults, but we can expect it to have a profoundly negative impact on health outcomes for years to come. A recent news report, for instance, suggested that the 20 percent rise in deaths from Alzheimer’s disease and dementia over this past summer may be connected, at least in part, to social isolation. AARP reports that some states have even begun listing “social isolation” or “failure to thrive” as a cause or contributing factor on the death certificates of some long-term care residents.
Added to this heartbreaking news, there is the ever-present dimension of racial inequity. While we still need to better understand all the ways social isolation associated with the pandemic has affected older adults of color, two facts suggest they have experienced disparate outcomes. First, COVID’s devastating impact on communities of color – particularly among Black people – is well-documented. Second, some suggest that even though Black older adults are less likely to live alone than are their white counterparts, other common experiences flowing from systemic racism accumulated over a lifetime may intensify their social isolation.
While many of us have – with fits, starts and bumps – shifted to a life lived largely online through Zoom meetings, FaceTime calls and even telehealth appointments, this is far from true for older adults. As a group, older adults tend to have lower rates of access to technology. And even when they do have access to the necessary devices, many older adults lack the training or experience needed to use them effectively. Additional barriers include hearing loss (which affects nearly two-thirds of those over 70) or impaired vision (13.5 percent of those over 65). All of these factors work against technology being a ready tool for reducing social isolation.
While the statistics paint a grim picture, it turns out that older adults may be more resilient than we are often led to believe. A recent article in Kaiser Health News by Judith Graham, a journalist specializing in issues of aging, points to some of the protective factors that may actually alleviate the risk of social isolation. For instance, older adults tend to be better able to regulate their emotions and manage stress than those who are younger. And a lifetime of experience, perspective and wisdom may help them cope with difficult times.
Still, the crisis in social isolation demands action, and the pandemic has spurred an enormous amount of creativity, especially among community-based organizations, to reach and engage older adults. A recent National Association of Area Agencies on Aging (n4a) summit hosted by their National Resource Center for Engaging Older Adults highlighted strategies from across the country. These included relying on “old-school” methods such as the telephone and “snail mail,” as well as:
- Making broader use of social isolation screening tools including one developed by the Maryland Living Well Center for Excellence and administered by professionals such as community health workers.
- Providing older adults with easy-to-use technology (e.g., pre-programmed tablets), training and ongoing support.
- Handing out Uber Eats gift certificates to older adults to order a meal delivery and then have a virtual chat with a volunteer over dinner.
- Hosting “tele-town halls” to offer community updates and information on important topics.
- Reaching out to family caregivers to offer them support in addition to that provided to the older adults they care for.
Beyond these specific ideas, one of the most powerful and resonant messages from speakers was to tailor all approaches to specific communities and make sure they are culturally relevant. This means developing meaningful partnerships and sharing of resources with trusted community-based organizations. These organizations are invaluable assets because they know their communities best, and they (literally and figuratively) “speak the same language.”
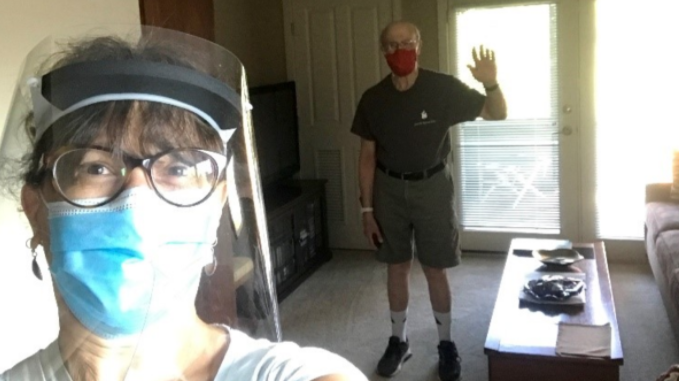
Seven months into the pandemic, I consider my father among the fortunate. Having only recently acquired a smart phone before the pandemic hit, he slowly but surely learned how to regularly text with me and my sister and how to participate in video calls and activities conducted over Zoom. And as the state’s COVID case numbers declined over the summer, his building eased many of the restrictions, so he was able to return to dining with other residents and attending events, all adjusted to meet stringent COVID safeguards. I was even able to visit him briefly in his apartment last month…albeit wearing a mask, plastic face shield and staying six feet apart. My Dad, like so many other older adults, has shown remarkable perseverance and resilience, reserves they will have to continue drawing upon as we move through a fall and winter in which the pandemic shows no signs of letting up.
The opinions expressed in this article are those of the author and do not necessarily reflect those of the Diverse Elders Coalition.